When comparing therapeutic potency, Suboxone and Subutex demonstrate identical strength at equivalent buprenorphine doses, with neither medication proving inherently stronger. The key distinction lies in Suboxone’s inclusion of naloxone, which provides critical abuse-deterrent properties absent in Subutex. You’ll experience similar clinical efficacy with both medications when taken as prescribed, though individual physiological responses may vary. Understanding the seven fundamental differences between these medications will help inform your treatment decisions.
Chemical Composition: Understanding Active Ingredients
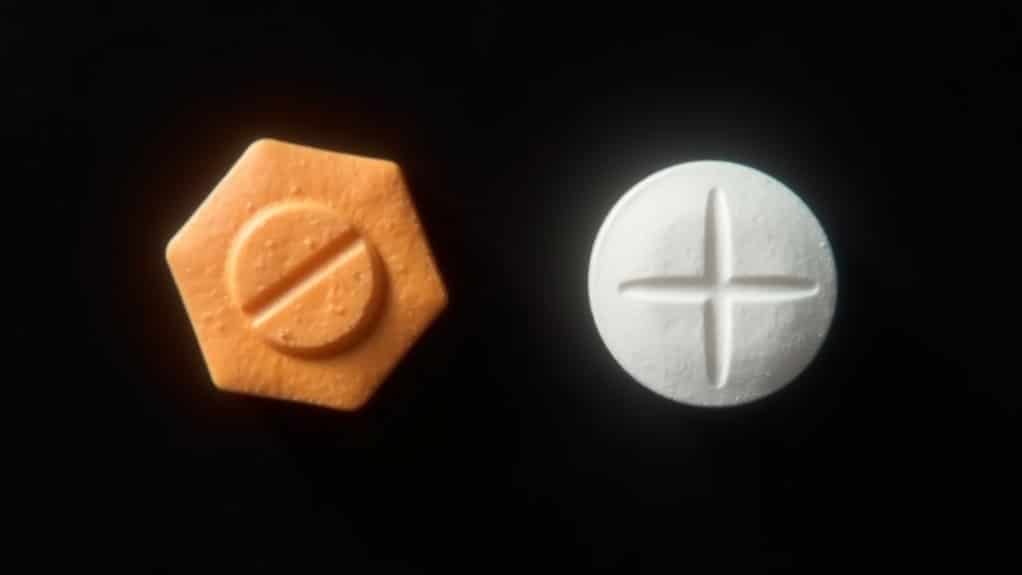
The fundamental distinction between Subutex and Suboxone lies in their active pharmaceutical ingredients. Subutex contains only buprenorphine HCl (C₂₉H₄₁NO₄), while Suboxone combines buprenorphine with naloxone. Subutex is available as an uncoated oval tablet in both 2 mg and 8 mg strengths. As part of a comprehensive treatment program, Subutex helps patients manage opioid dependence and withdrawal symptoms.
You’ll find that buprenorphine’s molecular structure includes specific cyclopropylmethyl and methoxy groups that enable its partial mu-opioid receptor agonist properties. Due to its unique properties, buprenorphine demonstrates a ceiling effect when taken in higher doses.
The chemical properties of these medications differ greatly in their therapeutic mechanisms. In Subutex, buprenorphine acts alone as a partial agonist, with dosing calculated based on the buprenorphine base equivalence. Meanwhile, Suboxone’s addition of naloxone introduces an opioid antagonist component that actively blocks full agonist effects when misused. This key difference in composition directly impacts their abuse potential and clinical applications in opioid dependence treatment.
Strength and Potency Comparison

Fundamentally, Suboxone and Subutex exhibit identical therapeutic potency when comparing equivalent buprenorphine doses, as both medications rely on buprenorphine’s partial mu-opioid agonist properties for their clinical effects. Both medications are administered under supervision when starting opioid addiction treatment.
Your treatment outcomes will depend more on proper dosing, individual physiology, and adherence rather than medication choice. Clinical studies haven’t demonstrated superiority in potency between these formulations when prescribed at equivalent buprenorphine doses. The main difference is that Suboxone deters abuse through its added naloxone component. The effects last 24 hours with either medication when taken as prescribed.
You’ll find that the receptor binding and partial agonist activity remain consistent across both formulations, regardless of Suboxone’s supplementary naloxone component. While their delivery methods differ Subutex as sublingual tablets and Suboxone as films these variations don’t affect the medications’ inherent strength. The pharmacokinetic profile and therapeutic window for opioid receptor modulation stay uniform between both options.
Safety Features and Abuse Prevention

While both medications effectively treat opioid dependence, Suboxone’s incorporation of naloxone provides critical abuse-deterrent properties that Subutex lacks. Under regulatory oversight, Suboxone’s dual-compound formulation actively blocks euphoric effects when misused, substantially diminishing diversion risks and medication availability on illicit markets. The ceiling effect of buprenorphine in both medications helps limit overdose potential, though Suboxone offers additional protection. Sublingual films make Suboxone easier to administer and more difficult to tamper with compared to Subutex tablets. Medical providers typically recommend Suboxone as the preferred choice for most patients seeking long-term recovery.
| Safety Feature | Suboxone | Subutex |
|---|---|---|
| Abuse Deterrent | Naloxone prevents injection/snorting | No built-in deterrent |
| Overdose Protection | Augmented through naloxone blocking | Limited protection |
| Home Use Safety | Preferred for unsupervised administration | Requires strict monitoring |
| Relapse Prevention | Higher barrier against misuse | Increased vulnerability |
You’ll find Suboxone’s built-in safeguards make it the preferred choice for long-term maintenance therapy, particularly in outpatient settings. Its formulation reduces overdose risks while maintaining therapeutic efficacy, offering superior protection against potential misuse compared to Subutex’s single-compound design.
Side Effects and Health Considerations
Understanding the side effect profiles of Suboxone and Subutex is pivotal for making informed treatment decisions, as both medications share common effects while maintaining distinct safety characteristics.
When comparing their risk levels, you’ll find that Suboxone’s naloxone component provides supplementary safeguards against misuse, though both medications can produce similar therapeutic outcomes under proper medical supervision.
Both medications may cause dry mouth and drowsiness, along with other common side effects that patients should monitor closely.
Pregnant women typically receive Subutex as the safer option during treatment due to its single active ingredient.
You’ll need to carefully weigh the potential side effects against the benefits of each medication, considering factors such as your individual health status, treatment goals, and risk factors for substance misuse.
Common Side Effect Patterns
Both Suboxone and Subutex exhibit distinct yet overlapping side effect patterns that stem from their primary active ingredient, buprenorphine. You’ll typically experience shared effects like constipation, dizziness, and drowsiness due to opioid receptor activation, though these vary based on drug interactions and medical history factors.
Suboxone’s unique side effect profile includes mouth numbness from its sublingual film and increased sweating associated with naloxone’s presence. In contrast, Subutex commonly presents with chills and anxiety, potentially requiring additional psychiatric monitoring.
Gastrointestinal patterns differ particularly between the medications – Suboxone users report more severe constipation, while Subutex patients may experience diarrhea. Neurological effects include blurred vision and concentration difficulties, with Suboxone users especially affected due to naloxone’s inhibitory properties.
Safety Profile Differences
Due to their distinct pharmacological compositions, Suboxone and Subutex present markedly different safety profiles in opioid dependence treatment. You’ll find Suboxone offers heightened protection against misuse through its naloxone component, which triggers severe withdrawal symptoms if injected. Both medications can cause dental complications, though Subutex shows a higher correlation with oral health issues.
| Safety Aspect | Suboxone | Subutex |
|---|---|---|
| Abuse Deterrence | High (naloxone) | Limited |
| Overdose Risk | Lower | Higher |
| Pregnancy Safety | Lower NAS risk | Higher NAS risk |
| Monitoring Needs | Relaxed | Strict |
| Emergency Response | May block other opioids | No interference |
It’s essential to note that both medications require careful hepatic monitoring and pose risks when combined with benzodiazepines. Your healthcare provider will consider these safety differences when determining the most appropriate treatment option.
Risk Level Comparison
Three distinct risk categories differentiate Suboxone and Subutex in clinical practice: side effect manifestation, physiological impact, and misuse potential.
While both medications share common adverse effects like headache and constipation, Subutex presents unique risks including chills and respiratory issues. Suboxone’s distinct profile includes dizziness and oral numbness, with notable GI impacts.
You’ll find higher diversion and misuse rates with Subutex due to its single-agent composition lacking naloxone’s protective effects. The overdose and relapse risks increase considerably when either medication is combined with alcohol or other substances.
Physiologically, both drugs exhibit a ceiling effect limiting opioid receptor activation, though Subutex shows enhanced efficacy in early withdrawal management. Suboxone’s naloxone component reduces injection risk but may precipitate withdrawal if misused.
Treatment Applications and Recovery Phases
Throughout the continuum of opioid dependence treatment, Subutex and Suboxone serve distinct therapeutic roles aligned with specific recovery phases. Subutex proves most valuable during early stabilization and detoxification, facilitating acute withdrawal management under close supervision. Clinical data shows that withdrawal side effects occur in 16% of Suboxone users compared to 9.7% of Subutex users. Close medical supervision is especially important for pregnant women using Subutex.
Subutex and Suboxone play unique roles in opioid treatment, with Subutex specializing in early recovery and withdrawal management.
Meanwhile, Suboxone excels in long-term maintenance therapy with ongoing dosage adjustments and behavioral therapy incorporation.
- Subutex enables rapid stabilization during short-term detox protocols lasting under 4 weeks
- Suboxone’s abuse-deterrent properties support sustained outpatient treatment with reduced monitoring requirements
- Both medications require integration with evidence-based behavioral interventions for ideal outcomes
- Treatment duration varies considerably: Subutex for weeks during induction, Suboxone potentially for months to years
The selection between these medications depends on your treatment phase, risk profile, and specific clinical circumstances, with safety and efficacy guiding the therapeutic approach.
Medication Forms and Administration Methods
While both medications contain buprenorphine as their primary active ingredient, Suboxone and Subutex vary considerably in their formulations and administration protocols. Suboxone includes naloxone as an abuse deterrent and comes in both film and tablet forms, while Subutex is available only as sublingual tablets without naloxone.
You’ll need to place these medications under your tongue or, with Suboxone films, inside your cheek. Proper dosage placement is vital – you must allow complete dissolution without swallowing, eating, or drinking. For multiple doses, position films side by side, adding subsequent doses only after the previous ones dissolve. The dissolution time directly impacts bioavailability, so maintaining the medication’s position is indispensable. Remember, you’re prohibited from altering these dosage forms by cutting or manipulating them in any way.
Prescription Guidelines and Availability
Beyond the physical administration protocols, accessing Suboxone and Subutex requires traversing specific prescription guidelines established by regulatory authorities. Physicians must complete specialized training and certification before prescribing either medication, with strict prescription window limits enforced to prevent misuse. Telehealth services now make these medications more accessible to patients seeking treatment from home.
Strict regulatory oversight governs access to Suboxone and Subutex, requiring specialized physician certification and enforced prescription limitations to ensure proper use.
Key prescription and availability factors include:
- Provider training requirements mandate completion of approved certification programs before prescribing privileges are granted
- Regular monitoring through toxicology screening and in-person evaluations dictates continued prescription eligibility
- Suboxone remains the preferred frontline treatment due to its abuse-deterrent formulation containing naloxone
- While Subutex’s brand formulation was discontinued in 2017, generic buprenorphine alternatives remain available for specific patient populations
Treatment protocols emphasize close medical supervision during induction, with ongoing adherence to structured maintenance programs essential for therapeutic success. Both medications are classified as Schedule III controlled substances that require careful oversight due to their potential for physical dependence.
Call Now and Start Your Recovery Today
Frequently Asked Questions
Can Pregnant Women Safely Take Suboxone or Subutex During Pregnancy?
Yes, you can safely take either Suboxone or Subutex during pregnancy, as clinical studies show no significant fetal development risks with either medication. Both options effectively manage opioid use disorder while protecting maternal and fetal health.
While your baby may experience prenatal withdrawal symptoms after birth, these are manageable under medical supervision. Your healthcare provider can help determine which medication is best based on your specific needs and circumstances.
How Long Should Patients Wait After Using Opioids Before Starting Either Medication?
You’ll need to wait different periods based on your last opioid use before starting buprenorphine induction. For short-acting opioids like heroin, wait 12-24 hours and confirm you’re experiencing moderate withdrawal symptoms (COWS score ≥6).
For long-acting opioids like methadone, wait 36-72 hours. Appropriate dosing guidelines require observable withdrawal symptoms including pupil dilation and physical discomfort to prevent precipitated withdrawal during the induction phase.
What Happens if You Drink Alcohol While Taking Suboxone or Subutex?
You shouldn’t combine alcohol with Suboxone or Subutex, as these opioid combinations can be life-threatening. The alcohol interactions amplify CNS depression, leading to dangerous respiratory suppression and increased overdose risk.
You’ll experience intensified side effects, including severe sedation, cognitive impairment, and potentially fatal respiratory failure. Even moderate alcohol consumption can trigger dangerous complications when combined with these medications.
Emergency medical intervention may be necessary if accidental co-ingestion occurs.
Can You Switch Between Suboxone and Subutex During Treatment?
Yes, you can switch between Suboxone and Subutex under medical supervision. Your healthcare provider will monitor your movement closely, as frequent dose adjustments may be necessary.
Most patients can maintain their current buprenorphine dosage during the switch, though some require fine-tuning. Relapse prevention strategies and compliance monitoring are essential during this transition.
You’ll need regular follow-up appointments in the primary few weeks to guarantee ideal therapeutic response and manage any adverse effects.
Do Insurance Companies Typically Cover Both Medications Equally?
You’ll find that insurance coverage levels typically differ between Suboxone and Subutex. Most major insurers prioritize Suboxone coverage, particularly its generic versions, while Subutex coverage is often more restricted.
Prior authorization requirements exist for both medications, but they’re generally more stringent for Subutex. Since the introduction of generics, you’ll notice that insurers have moved in the direction of covering generic buprenorphine-naloxone combinations over buprenorphine-only formulations like Subutex.






