Subutex is often preferred over Suboxone in clinical practice due to its simpler buprenorphine-only formulation, which allows for easier dose adjustments and fewer complications during early treatment. You’ll find it’s particularly beneficial during pregnancy and for patients with naloxone sensitivities. The medication’s cost-effective generic options can save you $200-300 monthly compared to brand-name alternatives. Understanding the key differences between these medications will help guide your ideal treatment choice.
Understanding the Key Differences in Drug Composition
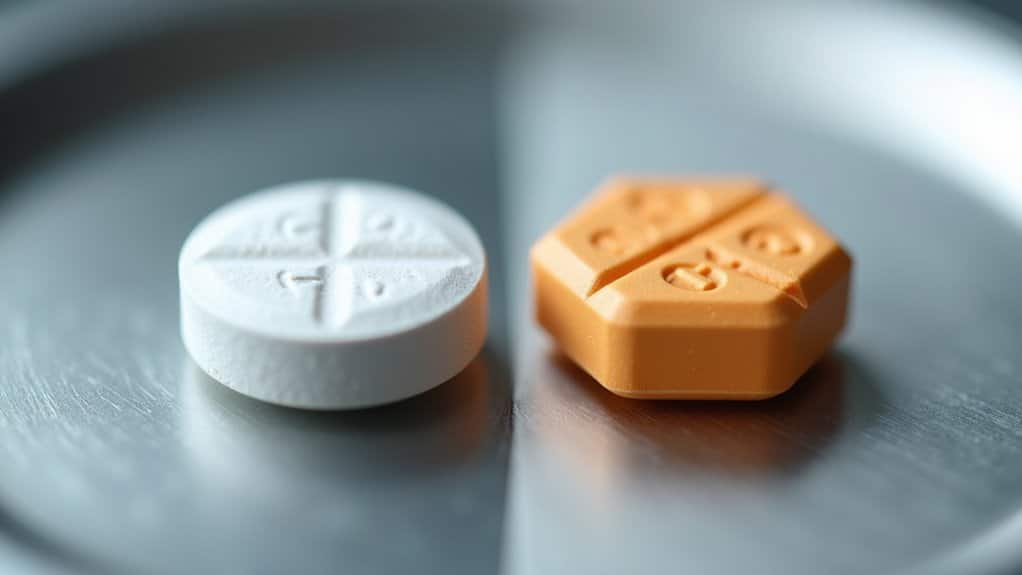
While both medications are used to treat opioid dependence, Subutex and Suboxone differ considerably in their chemical composition. Subutex contains only buprenorphine, a partial opioid agonist, while Suboxone combines buprenorphine with naloxone, an opioid antagonist. This medication formulation distinction greatly impacts their clinical applications and safety profiles. Medical supervision required makes Subutex the preferred choice in clinical settings like detox centers.
In terms of dosage administration, you’ll find Subutex available as a sublingual tablet that dissolves under your tongue. Suboxone, however, comes as either a sublingual film or buccal form that you’ll place between your cheek and gum. The inclusion of naloxone in Suboxone serves as an abuse deterrent, triggering withdrawal symptoms if the medication is injected, while having minimal impact when taken as prescribed. Subutex is often preferred during pregnancy since it lacks the naloxone component. It’s worth noting that while Subutex has been discontinued in the United States, it remains available as generic buprenorphine tablets.
Cost-Effective Treatment Options for Patients

When considering medication-assisted treatment, you’ll find significant cost differences between brand-name and generic versions of both Subutex and Suboxone. Generic buprenorphine (Subutex) offers monthly savings of $200-300 compared to brand-name options, while insurance coverage can further reduce out-of-pocket expenses. Available as sublingual tablets, buprenorphine provides a convenient administration method for patients starting treatment. Since buprenorphine acts as a partial agonist opioid, it helps control cravings without producing the intense high of full opioids. Recent data shows that this treatment approach is highly effective, with buprenorphine treatment being a proven method to help reduce opioid overdose deaths. Your healthcare provider can help evaluate insurance benefits and discount programs to determine the most cost-effective treatment path based on your specific situation.
Generic Options Save Money
The availability of generic Subutex offers significant cost advantages for patients seeking medication-assisted treatment for opioid use disorder. With greater generic medication availability, patients can access treatment at substantially lower costs compared to brand-name Suboxone. Treatment affordability becomes an essential factor in long-term recovery success and medication adherence. Both medications now have lower cost generic versions available to help patients access treatment.
Generic Subutex typically costs $160-$450 monthly, while Suboxone ranges from $200-$600, representing significant savings for patients managing chronic treatment needs.
Insurance providers often prioritize coverage for generic medications, making Subutex a more accessible option with fewer prior authorization requirements.
Initial prescription discounts for generic Subutex can save patients $200 or more, compared to Suboxone’s typical $50 savings, enabling more patients to begin and maintain their recovery process.
Insurance Coverage Versus Pricing
Insurance coverage variables profoundly influence treatment costs when comparing Subutex and Suboxone options for opioid use disorder management. You’ll find that Subutex often has a simplified billing process due to its monotherapy formulation, potentially reducing your out-of-pocket expenses through lower copays and favorable coinsurance rates. Major health insurance providers like Aetna, Blue Cross Blue Shield, and Humana typically cover both medications as part of their prescription drug benefits. Primary care providers may need to submit a prior authorization before insurance will approve coverage.
Your plan formulary positioning can drastically impact cost differences between these medications. The partial opioid agonist medication effectively manages withdrawal symptoms while keeping costs lower than combination drugs. Subutex may require fewer prior authorizations and face less stringent utilization restrictions, making it more accessible in certain insurance plans. You might encounter lower provider charges for Subutex treatment, and some insurers waive specific requirements for special populations like pregnant patients or those with comorbid conditions. It’s worth noting that your insurance plan’s deductible structure and out-of-pocket maximums could make Subutex more cost-effective in your specific situation.
Optimal Medication Choice During Early Recovery

Selecting the appropriate medication during early opioid recovery requires careful consideration of three key factors: patient tolerance, withdrawal risk, and supervision level. When evaluating Subutex versus Suboxone, clinicians often prefer Subutex for initial treatment due to its simpler formulation and reduced risk of complications.
During supervised inpatient care, Subutex’s absence of naloxone allows for faster dose escalation while minimizing precipitated withdrawal risks. The medication effectively deceives the brain’s receptors while providing therapeutic benefits with fewer intervention requirements. In specific cases like pregnancy or allergies, Subutex becomes the primary treatment choice. Patient preference and ongoing monitoring influence success rates, with Subutex’s tablet form potentially improving early compliance compared to films. High-tolerance patients benefit from Subutex’s stepwise dosing capabilities, enabling gradual stabilization before shifting to Suboxone’s abuse-deterrent properties.
This strategic approach optimizes treatment adherence while providing flexibility for individualized care plans, particularly during the critical early phase of recovery.
Managing Safety and Risk Considerations
When evaluating safety protocols for opioid dependence treatment, managing risks requires careful consideration of both medication formulations’ distinct properties. Subutex’s buprenorphine-only composition offers key advantages in reducing withdrawal severity during induction, particularly for patients with uncertain opioid tolerance levels. While Suboxone’s naloxone component helps prevent injection misuse, treatment preference factors often favor Subutex during early stabilization phases.
Subutex enables smoother dose adjustments without antagonist interference, while Suboxone provides built-in abuse deterrence. Patients starting treatment typically begin with a dose of 4 mg buprenorphine. Both medications require similar liver function monitoring and caution with other CNS depressants. For patients using multiple substances, you’ll want to conduct a thorough risk-benefit analysis, as Subutex may simplify management in complex cases.
Patient Tolerance and Side Effect Profiles
When considering Subutex versus Suboxone, you’ll find that Subutex’s absence of naloxone eliminates specific side effects like skin reactions and potential withdrawal complications that some patients experience with Suboxone. Your physical comfort during treatment may improve with Subutex due to steadier receptor occupation and fewer medication-induced fluctuations in symptoms. Subutex can be particularly beneficial as it is typically used in treatment facilities.
While both medications process through your liver, Subutex’s single-agent formulation can offer a more straightforward monitoring approach for patients with hepatic concerns. Both medications contain buprenorphine as treatment to help manage opioid addiction effectively.
Reduced Naloxone Side Effects
Because Subutex contains only buprenorphine without naloxone, it offers a simplified side effect profile compared to Suboxone’s dual-drug formulation. You’ll find greater medication versatility and dosing personalization options without naloxone’s potential complications. The absence of naloxone reduces risks of withdrawal-like symptoms, particularly in patients with slower metabolism or hepatic impairment.
- Eliminates common naloxone-related side effects including sweating, vomiting, and constipation
- Reduces risk of respiratory depression during early treatment stages
- Minimizes potential drug interactions due to simpler pharmaceutical composition
The single-agent formulation provides more predictable pharmacodynamics, especially beneficial during initial opioid withdrawal management. This streamlined approach allows for precise dose adjustments while maintaining effective symptom control, making it particularly valuable for patients requiring careful medication management or those with complex medical histories.
Physical Comfort During Treatment
Patients dealing with opioid dependence often face critical decisions about physical comfort during treatment. When considering Subutex versus Suboxone, you’ll find that Subutex’s single-agent formulation can reduce potential side effects and improve patient accessibility during the induction phase.
The absence of naloxone in Subutex may decrease initial adverse reactions and allow for smoother dose adjustments. You’ll experience different levels of mouth discomfort depending on the formulation you choose. While Subutex tablets require sublingual dissolution, which might take longer, they can be preferable if you have dental sensitivity or difficulty managing films. The tablet form also offers precise dose control through splitting options, making it easier to tailor treatment to your needs. For patients with specific medical conditions, Subutex’s simpler composition often translates to better physical tolerance.
Liver Impact Considerations
Beyond physical comfort considerations, liver health plays a central role in medication selection and dosing strategies. When comparing Subutex to Suboxone, medication metabolism becomes particularly crucial for special populations with compromised liver function. Since Suboxone contains both buprenorphine and naloxone, it requires supplementary hepatic processing compared to Subutex’s single-component formulation.
Patients with pre-existing liver conditions, such as hepatitis C or cirrhosis, often tolerate Subutex better due to its simpler metabolic demands. Clinical monitoring reveals that liver enzyme elevations tend to be less pronounced with Subutex, particularly in measuring ALT and AST levels. For elderly patients or those with reduced hepatic capacity, Subutex’s single-ingredient composition allows for more straightforward dose adjustments and reduced risk of drug accumulation.
Historical Evidence and Clinical Success Rates
Decades of clinical evidence demonstrate the effectiveness of both Subutex and Suboxone in treating opioid dependence. Provider prescribing trends show Subutex’s 75% retention rate after 24 weeks, while counseling and therapy combined with medication yields superior outcomes.
| Metric | Performance |
|---|---|
| Retention Rate | 75% at 24 weeks |
| Treatment Success | 75% vs 0% placebo |
| Patient Satisfaction | 37.5% consistent |
| Compliance Rate | >60% in trials |
| Relapse Prevention | considerably higher |
You’ll find that historical data supports both medications’ efficacy, with Subutex showing particular strength in specific populations. Clinical success rates indicate that buprenorphine-based treatments are 1.8 times more effective than non-medicated approaches, while maintaining strong safety profiles. Patient outcomes consistently improve when providers match the appropriate medication to individual needs and contraindications.
Treatment Protocols and Medical Guidelines
Building on the established efficacy data, treatment protocols for both medications follow distinct medical guidelines that shape prescribing practices. You’ll find that prescriber preference often leans in the direction of Subutex in specific clinical scenarios where patient adherence has been established and naloxone’s antagonist effects aren’t medically necessary.
- Clinical protocols prioritize Subutex during early induction phases to assess opioid tolerance without naloxone interference
- Treatment guidelines support Subutex use in low-risk patients who’ve demonstrated consistent compliance and proper medication management
- Medical protocols favor buprenorphine-only regimens for flexible dose titration, especially in closely monitored settings
Current guidelines emphasize individualized treatment approaches, allowing for Subutex administration in scenarios where simplified dosing improves therapeutic outcomes and supports long-term recovery success through carefully monitored maintenance programs.
Frequently Asked Questions
Can Pregnant Women Safely Take Subutex During Their Pregnancy?
Yes, you can safely take Subutex during pregnancy. Research shows no significant fetal development concerns when using Subutex to treat opioid use disorder while pregnant.
It’s an FDA-approved medication that helps prevent withdrawal complications and reduces risks for both you and your baby. You can also continue Subutex while breastfeeding, as studies show minimal transfer through breast milk and no adverse effects on infants.
How Long Does It Typically Take to Completely Transition off Subutex?
Your shift off Subutex will require a personalized dose tapering schedule that typically spans several weeks to months. The exact timeline depends on your initial dose, length of use, and individual health factors.
You’ll work with your healthcare provider to gradually reduce doses while monitoring for withdrawal symptoms. To guarantee successful patient relapse prevention, you’ll need consistent medical supervision and support throughout the process.
Most patients complete the shift within 3-6 months.
Are There Specific Drug Interactions to Watch for With Subutex?
You’ll need to be particularly cautious about several key drug interactions with Subutex. Combining it with CNS depressants like benzodiazepines or alcohol can drastically/enormously/vastly increase respiratory depression risks.
You should also watch for increased liver toxicity risks when taking acetaminophen or certain antibiotics. Be aware that Subutex can cause adverse effects on sleep patterns, especially when used with sedatives.
Always inform your healthcare provider about all medications you’re taking.
What Happens if You Miss a Dose of Subutex?
If you miss a dose of Subutex, you’ll likely experience withdrawal symptoms within 24-48 hours due to buprenorphine’s half-life. You may notice physical symptoms like nausea, sweating, and muscle aches, along with psychological effects such as anxiety and cravings.
Don’t double up on doses to compensate this can affect medication interactions and safety. Instead, take your next scheduled dose and contact your healthcare provider to discuss proper dosing adjustments.
Can Subutex Be Prescribed by Primary Care Physicians or Only Specialists?
Your primary care physician can prescribe Subutex if they’ve completed the required DATA 2000 waiver training and certification. You’ll need to discuss maintenance treatment duration and medication dosage adjustments with your prescribing doctor, whether they’re a PCP or specialist.
While both can legally prescribe, some PCPs may refer complex cases to addiction specialists. Keep in mind that all prescribers must maintain current certification and follow federal guidelines for buprenorphine prescribing.






