Suboxone and Subutex both contain buprenorphine for treating opioid dependence, but you’ll find key differences in their formulations. Suboxone includes naloxone as an abuse deterrent, while Subutex contains only buprenorphine. You’ll encounter Suboxone in a tamper-resistant film form that dissolves between your cheek and gum, whereas Subutex comes as a sublingual tablet. Both medications require professional supervision, but Suboxone’s dual-action approach offers boosted protection against potential misuse. Understanding these distinctions can greatly influence your treatment choices.
Key Components and Active Ingredients
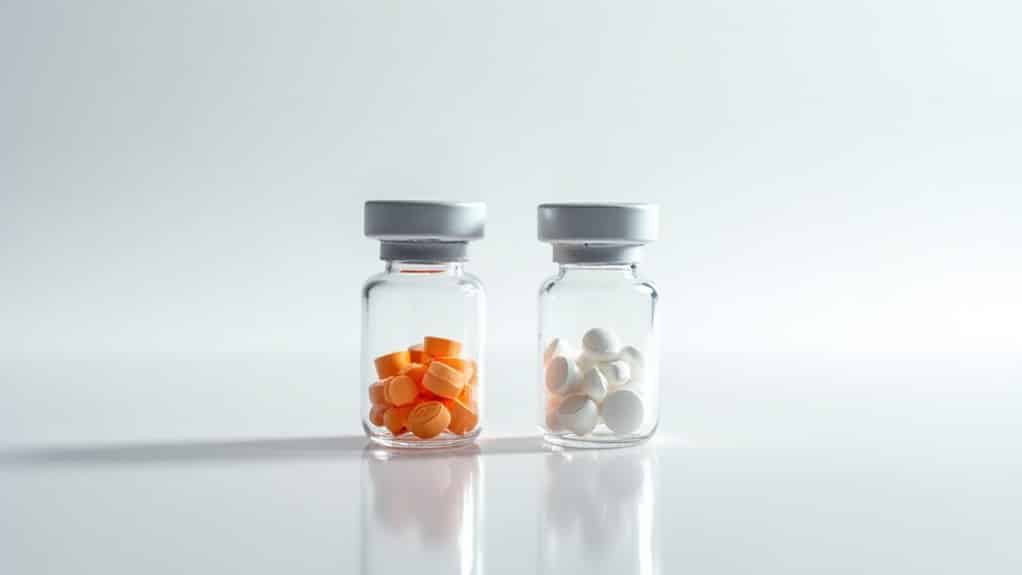
The key distinction between Suboxone and Subutex lies in their active ingredients and therapeutic composition. While both medications contain buprenorphine hydrochloride as a partial mu-opioid receptor agonist, Suboxone includes naloxone in a 4:1 ratio, serving as an abuse deterrent. These medications are proven to be highly effective when combined with counseling and behavioral therapy approaches.
You’ll find Suboxone available in 2mg/0.5mg and 8mg/2mg combinations, featuring orange hexagonal tablets with lemon-lime flavoring to boost dissolution properties. Subutex comes in 2mg and 8mg white oval tablets, containing only buprenorphine. Both medications require sublingual administration for ideal absorption rates, bypassing primary metabolism. The ceiling effect of buprenorphine means that taking higher doses will not produce stronger opioid effects. The tablets must be kept under the tongue until completely dissolved and should never be crushed, chewed, or swallowed.
The shared inactive ingredients include lactose, mannitol, and citric acid components, though Suboxone contains additional sweeteners and colorants to differentiate it from Subutex’s simpler formulation.
Safety Features and Misuse Prevention
Suboxone’s naloxone component actively blocks the euphoric effects if you attempt to inject or snort the medication, triggering immediate withdrawal symptoms that serve as a powerful deterrent against misuse. You’ll find extra safety features in Suboxone’s film formulation, which resists tampering through its specialized design that makes crushing or dissolving more difficult than traditional tablets. Both medications require close medical supervision to ensure safe treatment and monitor potential side effects. Medication-assisted treatment should always be combined with comprehensive therapy programs for the best treatment outcomes. Subutex contains only pure buprenorphine alone, making it a simpler and more affordable option than Suboxone. When taken as prescribed under the tongue, Suboxone’s naloxone remains inactive while the buprenorphine works effectively to prevent withdrawal and manage cravings, creating an inclusive safety profile that protects you during treatment.
Naloxone’s Protective Mechanism
Within Suboxone’s formulation, naloxone serves as a critical protective mechanism designed to prevent medication misuse and bolster patient safety. The drug’s receptor binding profile enables it to competitively attach to opioid receptors with higher affinity than other opioids, effectively blocking their effects without producing euphoria.
The drug’s single-use design and pre-measured formulations prevent tampering and overuse. Since naloxone only works in the presence of opioids and doesn’t produce psychoactive effects, there’s no incentive for recreational misuse. This built-in safety mechanism makes Suboxone a more secure choice for medication-assisted treatment.
You’ll find that naloxone’s protective features work through specific metabolic pathways, including hepatic glucuronidation, which creates non-toxic metabolites. It’s remarkably safe, with no adverse respiratory or CNS effects, even when other substances are present.
Film Vs Tablet Design
When comparing film and tablet formulations of buprenorphine medications, distinct safety features emerge that greatly impact misuse prevention. Film’s product form stability offers superior safeguards through its rapid dissolution and adhesive properties that prevent accidental swallowing.
You’ll find that films integrate tamper-resistant features in their drug product formulation, making extraction and injection considerably more difficult. The buprenorphine/naloxone combination provides an additional layer of abuse deterrence in these formulations.
The tablet design, while traditional, presents higher risks for manipulation. You can split tablets into smaller doses, crush them for alternative routes of administration, or attempt extraction for injection. In contrast, films’ standardized doses and cohesive structure resist tampering attempts. Their higher bioavailability when used correctly, combined with built-in deterrents against misuse, makes the film formulation a more secure choice for treatment delivery.
Withdrawal Prevention Features
Building upon the physical design safeguards, the pharmacological safety features of these medications offer distinct withdrawal prevention mechanisms. The pharmacokinetic properties of both formulations help manage withdrawal symptoms through controlled release, but Suboxone’s dual-action approach provides amplified protection against misuse.
Suboxone contains naloxone, which triggers withdrawal if injected, deterring intravenous abuse. Subutex’s pure buprenorphine composition requires stricter monitoring due to higher misuse potential. Studies show that room for improvement exists in current medication-assisted treatments, with over 50% of patients relapsing within 6 months.
Patient adherence factors improve with Suboxone’s antagonist component, discouraging deviation from prescribed use. Both medications’ partial agonist properties limit full receptor activation while blocking other opioids.
Suboxone’s combination formulation offers superior overdose protection through naloxone’s counteracting effects.
These withdrawal prevention features make Suboxone the preferred choice for most patients, though individual circumstances may warrant Subutex in specific cases.
Administration Methods and Daily Usage
Suboxone’s sublingual film dissolves between your cheek and gum, while Subutex tablets must be placed under your tongue for proper absorption. You’ll need to allow the medication to fully dissolve without swallowing, chewing, or drinking during administration to guarantee maximum effectiveness. Both medications require strict daily dosing schedules under medical supervision, though Suboxone’s film typically dissolves more rapidly than Subutex’s tablet form. Available doses range from 2 mg to 8 mg for Subutex tablets, providing options for individualized treatment plans.
Sublingual Film Vs Tablets
Understanding the key differences between sublingual films and tablets is essential for successful medication-assisted treatment. Regarding storage requirements and moisture sensitivity, both forms require specific handling methods to maintain their effectiveness.
Films come in dissolvable strips that you’ll place under your tongue, requiring dry hands during handling to prevent premature breakdown. Both medications contain active buprenorphine to help manage opioid withdrawals.
Tablets are solid forms that you’ll hold under your tongue until completely dissolved, needing clean handling techniques.
You can divide films into halves for dose adjustments, while tablets may need specific tools for splitting.
Store films in their original foil packaging to protect against moisture and maintain potency.
Keep tablets in secure, dry containers away from light and heat to prevent deterioration.
Daily Dosing Requirements
Proper daily dosing plays an essential role in successful Suboxone and Subutex treatment. You’ll typically start with an induction phase of up to 8mg on day one, before reaching a maintenance dose between 12-16mg daily. The length of daily dosage remains consistent due to buprenorphine’s long half-life, allowing for single daily administration.
| Phase | Dosage Range | Adjustment Schedule |
|---|---|---|
| Induction | 2-8mg | Day 1, split doses |
| Early Maintenance | 4-16mg | Every 3-7 days |
| Stable Maintenance | 12-24mg | Weekly as needed |
| Maximum Limit | 24-32mg | Increased monitoring |
Your dosage adjustment schedule will follow increments of 2-4mg based on your symptoms and tolerance. While standard guidelines cap doses at 24mg daily, some cases may require up to 32mg under close medical supervision.
Historical Development and FDA Approval
The development of modern opioid addiction treatments took a significant turn in 1966 when Reckitt & Colman synthesized buprenorphine as a pain reliever. Through strategic pharmaceutical development and patent expirations, the global market growth led to two distinct formulations targeting opioid dependence. Early research groups like the National Research Council dedicated extensive efforts to finding non-addictive alternatives to existing opioids.
Initially intended as an alternative to morphine, buprenorphine proved promising when researchers discovered its ability to negate opioid effects. The drug took nearly three decades before being used as a therapeutic treatment. Subutex, containing only buprenorphine, launched initially in France (1995). Suboxone followed with added naloxone to prevent misuse. Both medications received FDA approval in 2002. Reckitt secured 7-year market exclusivity through orphan drug status. DATA 2000 legislation enabled office-based prescribing.
This evolution marked a significant shift from traditional methadone clinic requirements to more accessible treatment options. You’ll find both medications demonstrated effectiveness in treating opioid dependence, though Suboxone became the preferred US formulation due to its abuse-deterrent properties.
Treatment Phases and Clinical Applications
When initiating opioid dependence treatment, clinicians must carefully consider the distinct applications of Suboxone and Subutex across different treatment phases. You’ll find Subutex commonly prescribed during the induction phase, as it contains only buprenorphine without naloxone, reducing the risk of precipitated withdrawal. Both medications have demonstrated they are more effective than placebo in managing opioid dependence.
Subutex’s single-ingredient formulation makes it ideal for initial opioid treatment, minimizing withdrawal risks during the critical induction phase.
For maintenance treatment, however, Suboxone becomes the preferred choice due to its abuse-deterrent properties from the added naloxone component. This approach has shown to improve treatment retention significantly when combined with comprehensive counseling programs.
In terms of pregnancy safety and special population management, Subutex has traditionally been the go-to selection for pregnant patients to minimize fetal exposure to naloxone. However, recent studies suggest Suboxone may be just as appropriate with proper monitoring.
Both medications effectively reduce neonatal abstinence syndrome compared to methadone, though treatment selection ultimately depends on individual patient factors and clinical circumstances.
Medication Forms and Delivery Systems
Both medications feature distinct delivery systems that directly impact their therapeutic effectiveness and abuse potential. Subutex comes as a sublingual tablet, while Suboxone offers sublingual and buccal film options. The film formulations dissolve faster and are specifically designed to reduce misuse potential.
Subutex tablets dissolve under the tongue, while Suboxone films adhere to either the cheek or beneath the tongue. Films provide quicker dissolution times compared to tablets, making diversion more difficult.
Brand name Suboxone remains widely available, while Subutex is now prescribed as generic buprenorphine. Medication costs tend to be lower for generic buprenorphine tablets versus brand name film variants. Film formulations resist extraction and tampering attempts more effectively than tablet forms.
The proper administration method is essential for both medications to guarantee ideal therapeutic benefits and prevent misuse.
Prescription Requirements and Availability
Obtaining either medication requires strict adherence to federal and state prescription protocols. You’ll need to receive treatment from a DEA-certified physician who’s completed specialized CSAT training and maintains proper documentation requirements. Treatment accessibility varies considerably between the two medications.
Suboxone offers broader insurance coverage and availability as the standard OUD treatment, while Subutex is typically reserved for particular populations like pregnant patients or those with documented naloxone allergies. Insurance coverage considerations often favor Suboxone due to its abuse-deterrent properties and established efficacy. Your geographic location may impact access, as rural areas frequently have fewer certified providers. In addition, if you’re a new patient, you’ll likely undergo supervised dosing initially, especially with Suboxone, to guarantee proper use and prevent misuse.
Side Effects and Medical Considerations
Understanding the side effects of Suboxone and Subutex treatment requires careful consideration of their distinct pharmacological profiles. While both medications share common effects like constipation and headaches, their unique formulations lead to different behavioral changes and individual tolerances.
Managing opioid dependency means weighing unique medication profiles, as Suboxone and Subutex can affect patients differently despite sharing core side effects.
Suboxone users frequently experience mouth numbness, increased sweating, and difficulty concentrating due to its naloxone component. Subutex patients commonly report psychological symptoms like anxiety and depression, along with physical effects such as chills and back pain.
Both medications require strict liver function monitoring and regular medical oversight. Suboxone’s naloxone component provides augmented protection against misuse and relapse. Subutex users need supplementary dental monitoring due to reported oral health complications.
Your healthcare provider will carefully evaluate these considerations to determine which medication aligns best with your specific medical needs and recovery goals.
Take the First Step Toward Recovery Today
Frequently Asked Questions
Can Pregnant Women Safely Take Suboxone or Subutex During Treatment?
Yes, you can safely take either Suboxone or Subutex during pregnancy when managing opioid use disorder. Both medications are considered initial treatments with proven prenatal health considerations and established medication safety concerns.
You’ll need consistent monitoring throughout your pregnancy, but research shows no significant long-term risks to your baby. Clinical guidelines support both options, though you should discuss your specific situation with your healthcare provider to determine the best choice.
How Much Do Suboxone and Subutex Typically Cost With Insurance?
With insurance, your costs for Suboxone or Subutex can vary considerably based on your coverage type. You’ll typically pay $10-12 copay amounts for generic versions, while brand-name Suboxone may cost $85-100 out-of-pocket.
Medicaid usually offers the lowest costs, especially for extended-release formulations. Your treatment duration will affect total expenses, and prior authorization requirements may impact coverage.
Commercial insurance copays tend to be higher than Medicaid or Medicare plans.
What Happens if You Drink Alcohol While Taking These Medications?
You shouldn’t drink alcohol while taking either Suboxone or Subutex due to dangerous interactions. Both medications contain buprenorphine, which can cause severe respiratory depression when combined with alcohol. You’ll face increased overdose risk, as the combination can slow your breathing to dangerous levels.
This interaction can lead to unconsciousness, coma, or death. Even small amounts of alcohol can create life-threatening complications when mixed with these medications.
Can You Travel Internationally With Suboxone or Subutex Prescriptions?
You can travel internationally with Suboxone or Subutex, but you’ll need to carefully follow customs regulations and drug laws for each country you visit or transit through. You must carry your original prescription, a doctor’s letter, and keep medications in their original containers. Contact embassies beforehand to verify specific requirements, as some countries require advance approval.
Always pack only personal-use quantities and maintain proper documentation throughout your excursion.
How Long Does It Take to Completely Taper off These Medications?
You’ll typically need 4-12 weeks to safely taper off buprenorphine medications, though this timeline can vary based on your individual needs. The most successful prescribed dose reductions follow a gradual tapering schedule, starting after a 28-day stabilization period.
Your healthcare provider will monitor your progress and adjust the taper speed according to your withdrawal symptoms. Some patients may benefit from longer tapers lasting several months to minimize discomfort and reduce relapse risk.






