You’ll find nitrous oxide contraindicated for several key conditions that demand careful screening. These include COPD exacerbations, pneumothorax, initial-trimester pregnancy, vitamin B12 deficiency, and certain blood disorders like pernicious anemia. You shouldn’t receive treatment if you have acute respiratory infections, recent head trauma, or compromised oxygen exchange. While generally safe under proper protocols, your healthcare provider must assess specific risk factors to guarantee appropriate administration. Complete understanding of contraindications requires thorough clinical assessment.
Key Respiratory Conditions That Prevent Safe Use
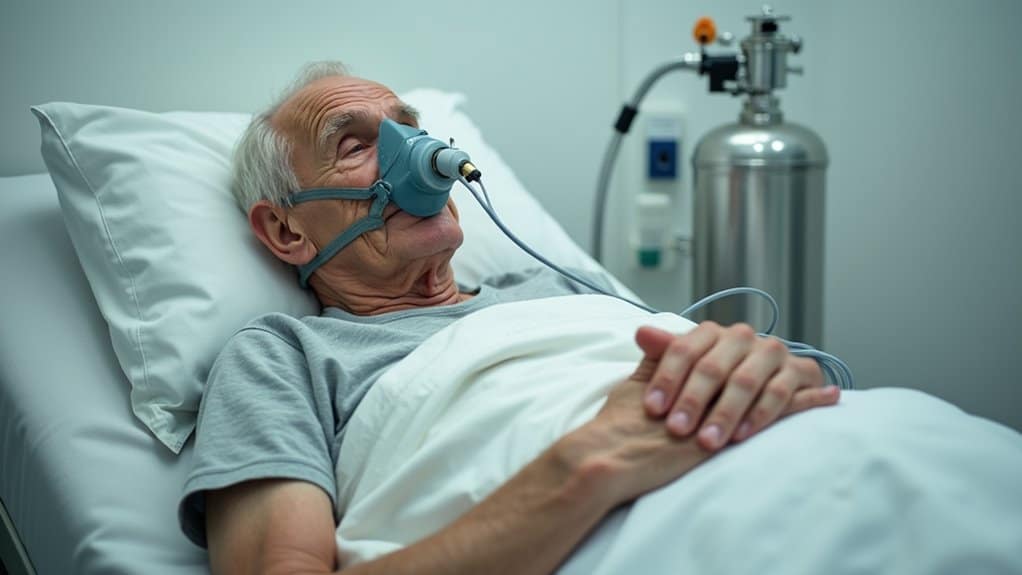
When evaluating patients for nitrous oxide administration, several respiratory conditions pose absolute contraindications due to their profound impact on gas exchange and ventilation. You’ll need to carefully assess COPD exacerbation risks, as these patients experience compromised oxygen exchange and heightened hypercapnia susceptibility. Their existing ventilation-perfusion mismatch can worsen with nitrous oxide exposure. The gas is most effective when patients can receive it through proper mask placement over both nose and mouth. For optimal safety, it’s recommended to conduct a 5-minute trial before proceeding with full treatment. Patients can feel confident knowing that nitrous oxide is heart and lung safe when proper screening protocols are followed.
Significant chest pathology complications, including pneumothorax, pulmonary contusions, and multiple rib fractures, present critical contraindications. These conditions severely disrupt normal gas distribution mechanisms and increase respiratory vulnerability.
Furthermore, emphysema patients face augmented risks due to air trapping and reduced functional reserve. In cases of respiratory muscle weakness, such as in MS patients with pulmonary involvement, you’ll find that impaired ventilation capacity and autonomic instability make nitrous oxide administration unsafe.
Pregnancy and Maternal Health Considerations
During pregnancy, you’ll need to follow strict trimester-specific safety protocols when receiving nitrous oxide, with initial-trimester exposure requiring heightened monitoring due to critical fetal development phases. Healthcare providers must maintain proper scavenging systems to minimize ambient exposure risks. The recommended blend is 50% oxygen and 50% nitrous oxide for safe administration during labor. Patients can experience fast-acting relief within 30 seconds of using the mask.
You must undergo mandatory B12 deficiency screening before labor-related nitrous oxide use, as deficiency can lead to adverse metabolic complications.
If you’re breastfeeding, you can safely receive nitrous oxide for dental procedures, as clinical studies show no significant transfer to breast milk and side effects typically resolve within 15 minutes post-administration.
Trimester-Specific Safety Guidelines
As pregnancy progresses through distinct trimesters, nitrous oxide safety guidelines require careful consideration of fetal developmental stages and maternal health factors. During early pregnancy, concerns about ovulation disruption and fetal neurodevelopment impacts make nitrous oxide exposure particularly risky, especially during critical organogenesis. NIOSH recommends that scavenging systems be used during any necessary nitrous oxide administration to minimize exposure risks. A comprehensive clinical review study found no significant increase in congenital abnormalities with short-term exposure. Second trimester procedures are often considered optimal timing for necessary dental work.
Primary trimester exposure should be strictly avoided due to potential interference with DNA synthesis and vitamin B12 metabolism during essential organ formation. Second trimester procedures using local anesthesia are preferred, as this period typically presents lower developmental risks. Third trimester administration isn’t recommended due to potential complications with preterm labor.
You’ll need to consult with both your dental provider and obstetrician before any procedure requiring anesthesia. While emergency procedures may warrant short-term exposure, alternative pain management strategies should be prioritized throughout pregnancy.
Breastfeeding and Recovery Timing
Since nitrous oxide exhibits rapid clearance properties in maternal circulation, breastfeeding mothers can safely resume nursing immediately after regaining full consciousness and physical stability. You’ll need to monitor your physical recovery metrics, ensuring adequate hand-arm coordination and absence of dizziness before attempting to hold your infant. While no mandatory waiting period exists, coordinate nutritional support during recovery with your feeding schedule. Local anesthetic safety has been extensively documented for nursing mothers, allowing for comfortable dental procedures without compromising breast milk quality. Research confirms that inhaled anesthetics transfer in clinically insignificant amounts to breast milk. The presence of natural nitric oxide in human milk means nursing mothers can be assured of its compatibility with breastfeeding.
If you’re experiencing temporary mobility limitations post-procedure, you should pump to maintain milk supply. Time your physical activity post procedure based on your recovery status, prioritizing infant safety during feeds. Inform your healthcare provider about your breastfeeding status to optimize anesthetic protocols, and consider pre-expressing milk if you anticipate delayed nursing due to procedural requirements.
Neurological Risk Factors and Warning Signs
While nitrous oxide exposure can affect multiple organ systems, its most significant impact manifests through distinct neurological warning signs that clinicians must monitor. You’ll need to watch for cognitive impairment patterns and cerebellar involvement effects, which often present as sensory ataxia and coordination problems. The abuse of nitrous oxide frequently leads to vitamin B12 deficiency and subsequent metabolic disruptions. Lower limb weakness with spasticity typically appears preliminary, accompanied by proprioceptive impairment and peroneal nerve deficits that disrupt your balance and motor control. Some patients exhibit extensor plantar reflexes during early neurological examination. Paresthesia in hands or feet often precedes motor deficits, while impaired vibratory sensation serves as a critical early indicator of dorsal column involvement. Central nervous system changes manifest as T2 hyperintensities in your cervical spine’s posterior region, creating characteristic “owl’s eye” or “snake-like” lesions visible on MRI. Dating back to the late 18th century, recreational use of nitrous oxide has a long history of causing neurological complications.
Blood Disorders and Metabolic Concerns
Understanding blood disorders and metabolic concerns proves critical when administering nitrous oxide, given its profound impact on vitamin B12 metabolism and hematopoiesis. If you’re predisposed to cobalamin deficiency risks or have methionine synthase pathway defects, you’ll face heightened susceptibility to adverse effects.
You’ll need stringent monitoring if you have conditions like pernicious anemia, MTHFR deficiency, or sickle cell anemia, as these represent strict contraindications. Your risk factors increase greatly if you’re vegan, elderly, or have conditions affecting B12 absorption, such as Crohn’s disease or post-gastrectomy status. You’ll require extensive blood work, including homocysteine levels and complete blood counts, particularly during extended exposure. Watch for warning signs like fatigue or weakness, as they may indicate subclinical B12 inactivation effects.
Emergency Medical Situations to Avoid Treatment
Recognition of emergency medical conditions requiring nitrous oxide avoidance proves essential for patient safety. You’ll need to carefully assess trauma patients for contraindications, especially those with gas-filled spaces or compromised anatomical structures.
If you’re evaluating head trauma or neurological emergencies, avoid nitrous oxide administration as it can worsen intracranial pressure and cerebral blood flow, particularly in patients with altered mental status or unconsciousness.
For abdominal trauma concerns, recognize that nitrous oxide can dangerously expand trapped gases, increasing risks of bowel perforation and fluid imbalance complications in cases of obstruction or pneumoperitoneum.
When managing decompression illness or post-diving emergencies, understand that nitrous oxide can exacerbate existing gas bubbles, complicating treatment outcomes and potentially worsening air embolism risks.
Patient Groups Requiring Special Assessment
Several distinct patient populations require thorough pre-assessment before nitrous oxide administration. You’ll need to carefully evaluate patients with nutritional disorders, particularly those following vegan diets or experiencing B12/folate deficiencies, as they face increased risks of neurological complications.
Patients with immunosuppression or complex medical histories, including recent surgeries or infections, demand specialized consideration due to potential gas expansion effects.
You must assess elderly patients with cognitive impairments, children under two years, and pregnant women in their first trimester with extra vigilance. Individuals with chronic respiratory conditions, such as severe COPD or pulmonary hypertension, require alternative treatment options.
Moreover, patients with acute intoxication, opioid dependence, or altered mental status present significant risks due to potential respiratory depression and compromised self-administration abilities.
Physical Health Restrictions and Limitations
Physical health conditions directly impact the safety and viability of nitrous oxide administration. You’ll need to carefully consider metabolic disorders, particularly MTHFR deficiency and B12 deficiency, which can affect how your body processes the gas. These conditions may require alternative approaches to chronic pain management.
If you have respiratory conditions or gas-filled spaces in your body, nitrous oxide can cause dangerous expansion effects, potentially complicating pneumothorax or bowel obstructions.
For those with vitamin B12 deficiency or MTHFR enzyme deficiencies, the gas can interfere with normal metabolic processes, leading to neurological complications.
During the initial trimester of pregnancy, nitrous oxide is strictly contraindicated due to potential teratogenic effects, requiring alternative anesthetic methods for any necessary procedures.
Time and Exposure Safety Guidelines
Safe administration of nitrous oxide requires strict adherence to established exposure limits and monitoring protocols. You’ll need to follow duration-specific regulations, particularly NIOSH’s recommended exposure limit of 25 ppm during anesthetic administration. This time-weighted exposure control differs from standard 8-hour workplace metrics.
To maintain safe exposure levels, you must implement proper engineering controls, including scavenging systems and demand valves with facemasks. Your facility’s ventilation system should complement these primary controls. You’ll need to conduct regular air quality testing to verify N₂O concentrations remain below threshold limits.
During procedures, guarantee patients maintain recumbent positioning and minimize talking. Always perform a 5-minute oxygen flush post-procedure to clear residual N₂O from equipment, and verify proper circuit bag expansion/contraction during patient breathing.
Mental Health and Behavioral Risk Factors
You’ll need thorough psychiatric screening before nitrous oxide administration, with particular attention to severe mental disorders, psychotic conditions, and current medication regimens.
Your history of substance use or addiction must be carefully evaluated, as nitrous oxide carries significant risks for individuals with prior substance abuse patterns.
Your emotional stability and current mental state require assessment, focusing on anxiety levels, trauma history, and potential triggers that could complicate sedation procedures.
Psychiatric Disorders Risk Assessment
When evaluating patients for nitrous oxide administration, psychiatric risk assessment remains critical due to the compound’s vital potential to exacerbate existing mental health conditions or precipitate new psychiatric symptoms. Understanding baseline personality traits and conducting thorough cognitive functioning assessments can help identify high-risk individuals.
- You’ll need to screen for schizophrenia, OCD, and bipolar disorder, as these conditions remarkably increase the risk of psychotic episodes and manic states during exposure.
- You must evaluate for active suicidal ideation and depression, as nitrous oxide can intensify emotional instability.
- It’s crucial to assess anxiety levels and previous psychotic episodes, since the drug’s NMDA antagonist effects can trigger severe psychiatric complications, including persecutory delusions and auditory hallucinations.
Addiction History Considerations
Patient addiction history warrants rigorous evaluation prior to nitrous oxide administration, as individuals with substance use disorders face heightened risks of adverse outcomes and dependency patterns. You’ll need careful screening for medicinal misuse patterns and coexisting health conditions, particularly given the drug’s rapid onset/offset cycle that reinforces addictive behaviors.
| Risk Factor | Clinical Concern | Monitoring Need |
|---|---|---|
| Polysubstance Use | Heightened respiratory depression | Continuous vital signs |
| Prior Dependencies | Accelerated tolerance development | Usage frequency checks |
| Current Recovery | Potential relapse trigger | Recovery plan adjustment |
| Behavioral History | Impaired decision-making | Enhanced supervision |
Your susceptibility to psychological dependence increases enormously if you’ve previously struggled with substance use, as nitrous oxide can activate similar neurochemical pathways. The compound risk of developing tolerance while managing existing recovery protocols requires specialized clinical oversight and tailored treatment approaches.
Emotional Stability Screening
Thorough emotional stability screening stands paramount before nitrous oxide administration, as mental health vulnerabilities can markedly impact treatment safety and efficacy. You’ll need expansive psychological assessment focusing on specific risk domains that could contraindicate treatment.
Monitor for elevated SCL-90 scores, particularly in anxiety, depression, and psychosis domains, as these conditions may intensify during administration and require specialized protocols
Evaluate behavioral patterns indicating concurrent substance use disorders, including hazardous use history and social/interpersonal dysfunction that could compromise treatment safety
Assess dissociative tendencies through CADSS-28 scoring, as heightened dissociative states may predispose patients to adverse reactions and risky behavior during administration
Your meticulous screening protocol should incorporate standardized assessments like HDRS-17 and MADRS to establish baseline emotional stability metrics before proceeding with treatment.
Frequently Asked Questions
Can I Drive Immediately After Receiving Nitrous Oxide Treatment?
You shouldn’t drive immediately after receiving nitrous oxide. The post-procedure recovery time typically requires 15-30 minutes of monitoring, during which you’ll need to remain at the dental office.
Potential side effects like residual sedation, altered perception, and delayed reaction times can impair your driving ability. You’ll need your dentist’s approval before leaving, and they’ll assess your alertness and coordination to verify you’re safe to operate a vehicle.
How Long Should I Fast Before Nitrous Oxide Administration?
For routine nitrous oxide administration, you should fast for 2 hours before your procedure. If you’ve eaten a light meal, this timeframe is generally sufficient. However, if you have preexisting medical conditions or recent injuries that might affect gastric emptying, your provider may recommend longer fasting periods.
If you’re receiving N2O combined with other sedatives, you’ll need to fast for 4 hours for solids and 2 hours for clear fluids.
Will Nitrous Oxide Affect My Existing Dental Fillings or Crowns?
You don’t need to worry about nitrous oxide affecting your existing dental restorations. The gas won’t compromise your dental restoration integrity, as it doesn’t chemically interact with filling materials, crowns, or other dental work.
While medical condition monitoring is essential before nitrous oxide administration, this focuses on respiratory and cardiovascular health rather than dental work. Your existing fillings and crowns will remain stable throughout the sedation process.
Does Smoking Before Nitrous Oxide Treatment Increase Any Risks?
Yes, smoking before nitrous oxide treatment drastically increases your risks. Recent nicotine use can cause nausea, vomiting, and impaired healing responses. You’ll face heightened complications, especially if you have underlying respiratory conditions.
When combined with nitrous oxide, smoking can trigger adverse cardiovascular reactions and reduce oxygen uptake. It’s essential that you disclose any tobacco use to your provider and follow their recommended cessation timeline before treatment.
Can I Receive Nitrous Oxide if I Have Seasonal Allergies?
You can generally receive nitrous oxide if you have seasonal allergies, but your provider needs to evaluate your current symptoms. If you’re experiencing significant nasal congestion, it might affect the delivery and effectiveness of the treatment since nitrous oxide is administered through a nasal hood.
Your immune system response and asthma management should be stable. Consider scheduling your treatment when allergy symptoms are minimal for ideal results.






